Periodontal disease is the scientific name used to describe gum disease. There are two common forms of periodontal disease. The first is called gingivitis, which is mild inflammation of the gums. The other, more serious, form of gum disease is called periodontitis, in which there is more severe inflammation of the gums, and the bone that holds the teeth in place begins to be gradually destroyed.
There are a number of ways to recognize whether you have periodontal disease or not. The most certain way to find out is of course to see your Dentist. Dr. Rosales, provides free consultations to all of our current, past, and future patients. Why wait for the disease to take effect when Dr. Rosales can examine your dental health and begin a preventative treatment. If Dr. Rosales sees that there is a chance of periodontal disease, he will have a digital x-ray taken to check the health of the bone that holds the teeth in place.
[one_third]
[/one_third]
[two_third last]
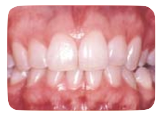
(Figure 1) Healthy gums are pink, firm, and tightly attached to the teeth. When flossing or brushing your teeth, they usually will not bleed. Keeping an active dental hygiene will allow your gum tissue to be healthy. Patients who brush their teeth at least twice a day and floss after each meal or prior to the end of the night, will see much better oral health. Finally, using the insurance benefits or simply arranging the “every-6-month-cleaning” will greatly keep your gums and teeth looking their best.
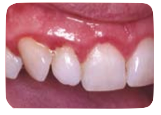
Gingivitis will develop when the teeth are not adequately brushed everyday and twice per day. Because of the lack of brushing, plaque builds up on the teeth next to the gums and the bacteria in the plaque will cause the gums to become inflamed and swollen (See Figure 2).
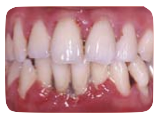
The gum inflation can become more severe causing the gums to detach from the root of the tooth. This creates a space between the gum and the tooth called a “pocket,” which is measured by the dentist with a probe. As the pocket worsens, the jaw bone holding the teeth in place gradually becomes destroyed. This process is typically painless and progresses very slowly. After a number of years and a large amount of the bone has eroded away, the tooth will start to become mobile or loose. (see Figure 3).
So what does periodontal disease have to do with diabetes?
In people with diabetes, there is an increased incidence of periodontal disease. We still don’t know the precise reasons why people with diabetes are more likely to suffer from periodontal disease. However, there are several factors which are important to consider:
- The immune system may not function properly in people with diabetes, thereby increasing the risk of periodontal disease.
- Damage to capillaries in the gums may reduce the blood supply to the gums, thereby limiting the actions of defense cells.
- Wound healing is impaired in diabetes, and therefore, healing in the gums is also reduced
[/two_third]
[clear]
What is the treatment for periodontal disease?
As with most diseases, prevention is better than a cure. Periodontal disease can generally be prevented by maintaining good oral hygiene (i.e. cleaning your teeth effectively).
Brush your teeth twice per day, for approximately 2-3 minutes each time. Be sure to brush every surface of the teeth, and particularly the point where the gum meets the tooth. The toothbrush should be positioned so the bristles contact the point where the gum meets the tooth at about a 45 degree angle. Use short back and forth strokes of the brush, with gentle pressure.
An electric toothbrush brush for most people is as effective as a manual toothbrush. They can also be useful if you have restricted movement. Make sure you clean in between the teeth using floss.
Sources: Diabetes Research and Wellness Foundation
